Written by MasterHealth Staff
Jump To Section
MS lesions are regions of demyelination within the central nervous system where the myelin sheath, the nerve coating responsible for conducting nerve signals, becomes damaged.
You can think of MS lesions like little scars that form around the myelin sheath. These scars result from inflammation brought on by the immune system, which is why MS is believed to be an autoimmune disease.
By following specific healthy diet and lifestyle interventions you can reduce the occurrence of MS lesions and their associated symptoms.
For more information on adopting a lifestyle and diet to fight MS, see The Wahls Protocol® by Dr. Terry Wahls, MD. and Wahls Diet: Mastering MS and Autoimmunity.
Brain lesions can form as a result of any trauma to the brain, either through external physical injury or internal injury. External injury could be caused by chemical exposure or infection, while internal causes could be due to stroke, reduced blood supply to an area of the brain, epilepsy, brain aneurysms, or a brain tumor.
Demyelinated MS lesions can mimic other conditions, including Guillain-Barre syndrome which is often caused by infection, and neuromyelitis optica and transverse myelitis which are both caused by long lesions within the spine. MS lesions are unique from other demyelinated lesions because they’re usually found within multiple areas of the central nervous system (CNS), and often have a unique appearance and location that sets them apart.
MS lesions are localized areas of demyelination within the CNS, which includes the brain, spine, and optic nerves. MS lesions can appear in the gray matter of the brain, but most often show up in the white matter, often positioned around the ventricles (fluid spaces) and the cortex, as well as the brainstem and cerebellum of the brain.
MS lesions will most often present in more than one region of the CNS – a feature which helps to confirm the diagnosis of MS.
MS lesions in the brain can often correspond with clinical symptoms. So a lesion in the cerebellum, which is responsible for balance and coordination, can sometimes cause difficulties in these functions.
Brain lesions mostly affect vision, hearing, speech, balance and spatial coordination, fine motor coordination, and cognition (including memory and information processing).
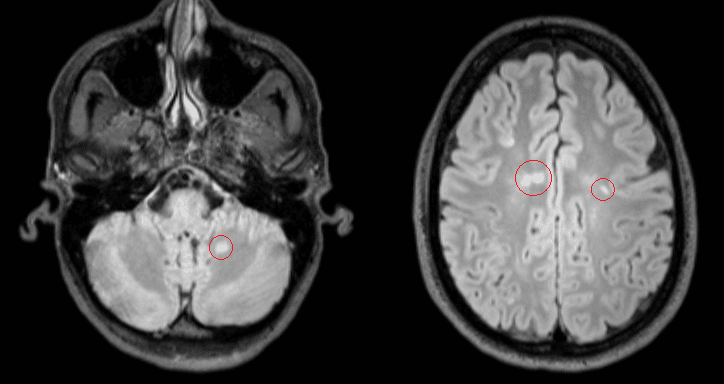
MS brain lesions can appear bright, dull or dark on MRI, and their appearance depends on whether the lesion is active, inactive, or disintegrated. Active lesions tend to appear as a bright oval on MRI when gandolinium, an injected contrast dye, is used. Without gandolinium, inactive lesions will appear darker.
MS lesions that seem to disappear on MRI have been found to be associated with worsened clinical disease outcomes and greater disability because the lesion and associated nerve have been dissolved into cerebrospinal fluid (CSF), indicating nerve atrophy. In these cases, the CSF permanently removes the damaged tissue along with other waste materials.
MS lesions on the spine can lead to greater disability, and tend to appear more commonly in people diagnosed with progressive forms of MS.
Symptoms associated with MS lesions on the spinal cord include muscle weakness, bladder and bowel incontinence, sensations of the skin (numbness, tingling, burning, electric shocks), limb paralysis and pain. Spinal lesions can also cause balance issues when they occur within the cervical spine (the neck).
A lesion can stay active and may cause symptoms for several days to weeks after the initial appearance of the lesion.
An MS lesion is considered ‘active’ when there is ongoing inflammation caused by the immune system. When the inflammation subsides, the lesion is considered to be ‘inactive’, but the nerve often remains demyelinated and damaged.
Some MS lesions have the potential to heal, but oftentimes they leave behind a scar where the lesion once was. Other times, lesions may not be able to heal because the cells responsible for myelin repair become damaged or die. In these cases, the lesions will be replaced by little black holes where the white matter has completely atrophied.
MS lesions that heal do so by a process called remyelination. Remyelinated lesions are called ‘shadow plaques’ in their earlier stages because they are neither active nor inactive lesions, and they appear different from undamaged tissue. And when remyelination is complete, the tissue may closely resemble healthy tissue.
Researchers have recently started to investigate potential therapeutic agents targeted at remyelination, and there are several natural interventions that may help.
We’ve done a deep dive into remyelination and myelin sheath repair, and the various ways you can naturally support the health of your myelin.














